Health Care Denied
Patients and physicians speak out about Catholic hospitals and the threat to women’s health and lives
Overview
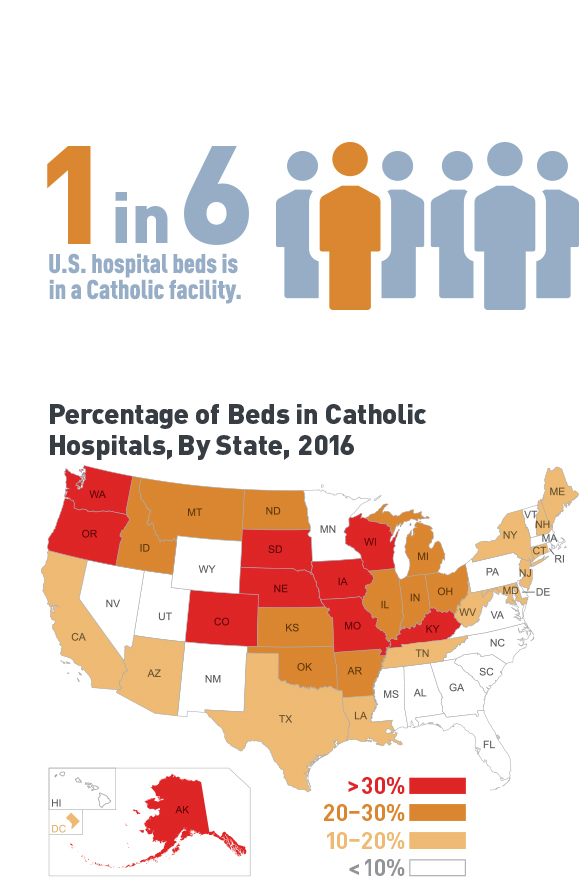
New reports from the ACLU and MergerWatch reveal that one in six hospital beds in the U.S. is in a facility that complies with Catholic directives that prohibit a range of reproductive health care services, even when a woman’s life or health is in jeopardy. In some states, more than 40 percent of all hospital beds are in a Catholic-run facility, leaving entire regions without any option for certain reproductive health care services. The ACLU’s report shares firsthand accounts from patients who have been denied appropriate care at Catholic hospitals, from health care providers forbidden from providing critical care because of the Directives, and from physicians at secular hospitals who have treated very sick women after they were turned away from a Catholic facility.
The Ethical and Religious Directives for Catholic Health Care Services, which are promulgated by the U.S. Conference of Catholic Bishops, set forth standards for the provision of care at Catholic health care facilities. The Directives prohibit a range of reproductive health services, including contraception, sterilization, many infertility treatments, and abortion, even when a woman’s life or health is jeopardized by a pregnancy. Because of these rules, many Catholic hospitals across this country are withholding emergency care from patients who are in the midst of a miscarriage or experiencing other pregnancy complications. Catholic hospitals also routinely prohibit doctors from performing tubal ligations (commonly known as “getting your tubes tied”) at the time of delivery, when the procedure is safest, leaving patients to undergo an additional surgery elsewhere after recovering from childbirth. Catholic hospitals deny these essential health services despite receiving billions in taxpayer dollars. Transgender and gender-non-conforming patients suffer the same and other, similar harms when seeking reproductive health care.

Report: Health Care Denied
This report shares firsthand accounts from patients who have been denied appropriate care at Catholic hospitals, from health care providers...
Source: American Civil Liberties Union
Top Report Findings
Looking to new data from MergerWatch, the ACLU report finds
- Today, one in six hospital beds in the United States is in a Catholic hospital.
- A total of 548 hospitals, or 14.5 percent of all short-term acute care hospitals in the U.S., comply with the Directives, either because they are owned by a Catholic health system or diocese, affiliated with a Catholic hospital or system through a business partnership, or are historically Catholic hospitals that continue to follow the Directives despite now being owned by a secular non-profit or for-profit health care system. This reflects an increase of 22% since 2001.
- In some places, such as Washington State, more than 40 percent of all hospital beds are in a Catholic hospital, and entire regions have no other option for hospital care;
- In ten states, more than 30 percent of all hospital beds are in Catholic facilities, and in nearly half the states, more than one in five hospital beds is in a Catholic facility.
Report Recommendations
- A statement from the Centers for Medicare and Medicaid Services (CMS) clarifying that all hospitals, regardless of religious affiliation, are required by federal law to provide emergency reproductive health care;
- A systematic investigation by CMS into violations by Catholic hospitals of federal laws requiring emergency care, and a commitment to taking all necessary corrective action where violations are found;
- Most importantly, a change in our public policies, to protect women in need of reproductive health services and the practitioners who are prohibited from providing this essential care.
Jennafer Norris
Jennafer and Jason Norris were shocked to learn in 2014 that Jennafer was pregnant after a rare birth control failure. At 30 weeks, her health took a severe downturn. She was admitted to Mercy Hospital Northwest Arkansas and diagnosed with fast onset of atypical preeclampsia, which caused symptoms ranging from blurred vision to excruciating headaches. Jennafer’s blood pressure was also extraordinarily high, putting her at great risk of a seizure or stroke. Everyone was terrified. Jennafer was scheduled to deliver by C-section, and she requested a tubal ligation at the time of the delivery—for obvious reasons, she could not risk getting pregnant again. But the hospital refused. While Jennafer’s physician was sympathetic, she explained with regret that she was bound by the Catholic hospital’s policy prohibiting sterilization. The only alternative, the hospital staff informed Jennafer, was to be treated at another hospital. The Norrises were outraged: The nearest hospital was 30 minutes away, Jennafer was in horrible pain and so dizzy that she could hardly see, and her medical team had warned her repeatedly that she could have a stroke or seizure at any moment. Jennafer and Jason decided that they could not risk it, and she went ahead with the delivery at the Catholic hospital.

Tamesha Means
Tamesha Means was 18 weeks pregnant with her third child when her water broke. She rushed to the nearest hospital, which is operated by Mercy Health Partners in Muskegon, Michigan. Because she was only 18 weeks along, the pregnancy was not viable. Ending the pregnancy would have been the safest course of action, but the hospital’s religious policies forbade it—so they gave Tamesha two Tylenol and sent her home without telling her that there was virtually no way she could give birth to a healthy baby. When Tamesha returned the next morning, she was bleeding, in severe pain, and showing signs of an infection; again, she was turned away. Even after she returned a third time, in excruciating pain, the hospital staff began filling out the discharge paperwork. It was only when Tamesha began to deliver that the hospital provided care. The baby died within hours.

Mindy Swank
Mindy Swank and her husband were thrilled to learn that they had a second child on the way. Their joy quickly dissipated, however, when Mindy’s water broke prematurely at 20 weeks and they learned through testing that the fetus, because of health conditions, could not survive. Waiting for Mindy’s body to complete the miscarriage on its own could expose her to infection and hemorrhaging; nevertheless, in accordance with the Directives, the Catholic hospital in Illinois where Mindy had received the genetic testing would not perform an abortion while there was still a fetal heartbeat.
For nearly two weeks, Mindy struggled with the emotional strain of continuing a pregnancy when she knew her baby could not survive. Then, one morning, she woke up bleeding. In a panic, Mindy and her husband rushed to their local hospital to ask them to complete the miscarriage. But that hospital also adhered to the Directives, and refused to induce labor. Mindy returned to that hospital multiple times over the next five weeks and was repeatedly turned away—without even being told that she could get the abortion if she went elsewhere. Finally, when she was 27 weeks pregnant and severely hemorrhaging, they induced labor. The baby died shortly after delivery.
Angela Valavanis
Angela Valavanis did not learn that her OB-GYN was prohibited from performing a tubal ligation at Presence Saint Francis Hospital in Evanston, Illinois, until she had already been in labor for three days and was being wheeled in for her C-section.

Jessica Mann
While Jessica Mann was pregnant with her third child in 2015, her doctors explained to her that because she had pre-existing brain tumors, another pregnancy could kill her. They highly recommended that she get a tubal ligation—a safe, effective, and extremely common form of contraception—to prevent another pregnancy. They also recommended that she have the tubal ligation at the same time as she delivered her baby to avoid the serious risk to her health that would be caused by having to undergo a second procedure after recovering from childbirth. But the hospital where Jessica planned to deliver her baby forbade her OB-GYN from providing this safe and effective care.

Related Content

What every family should know about their hospital
What important question should you be asking your hospital when you’re expecting?
Catholic Bishops Play Doctor With Pregnant Woman With Brain Tumor [BLOG]
The Rising Threat of Religious Hospitals Denying Women Medical Care [BLOG]
Angela Was Pregnant and Unable To Get the Health Care She Needed [VIDEO]